Choosing how to replace missing teeth is one of the most important dental-health decisions a senior in the United States may face. The choice affects chewing, nutrition, speech, facial appearance, jaw bone health, ongoing cost, and — most importantly — quality of life. Two of the most common options are dental implants (single implants or implant-supported prostheses) and dentures (partial or full). Dental Implants vs Dentures:
- Dental implants are a more durable, natural-feeling option that helps preserve jaw bone and often allows near-normal chewing, but they require surgery, a longer healing time, and a higher upfront cost. They can be the best long-term solution for medically suitable seniors who can afford or finance them.
- Dentures (traditional removable dentures) are the lower-cost, faster option that requires no major surgery and can restore appearance and basic chewing, but they generally do not stop bone loss, may require relines/replacements, and often feel less stable — which affects diet and comfort.
Below we expand on each aspect so you can compare like-for-like and make an informed choice.
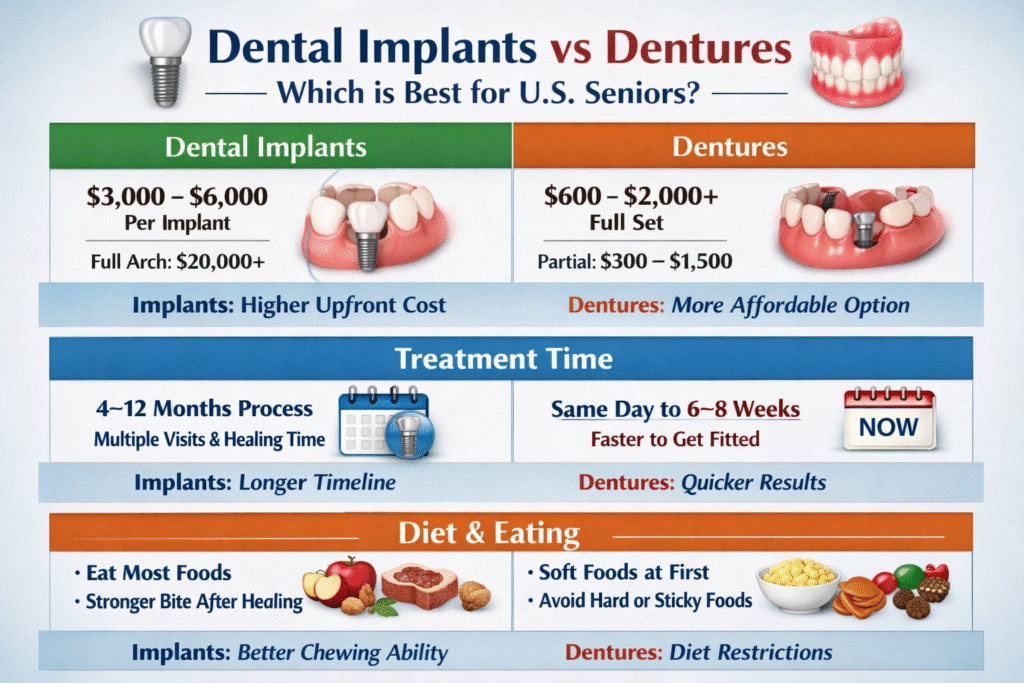
1) Dental Implants vs Dentures Cost — upfront and long term
Dental implants
- Typical U.S. cost (single tooth): about $3,000–$6,000 per implant (implant post + abutment + crown) as of recent pricing analyses. Full-arch implant solutions (e.g., “All-on-4” or implant-supported fixed bridges) can range widely — often $20,000–$50,000+ per arch depending on number of implants, materials, bone grafting, and clinic. These are national averages and vary by state, clinic, and complexity.
- Why so expensive: implants require surgical placement, CT scans or 3D planning, lab-made restorations, and often multiple visits. Bone grafts or sinus lifts raise cost further.
Dentures –
- Typical U.S. cost: $600–$2,000+ for a complete set of conventional removable dentures (economy to premium). Partial dentures cost vary by design (acrylic vs metal framework). Implant-retained snap-in dentures are in a hybrid cost zone because they combine implants with a denture (often $5,000–$20,000+ depending on number of implants).
Long-term economics –
- Upfront vs lifetime: Dentures are cheaper upfront but usually require relining every few years and replacement every 5–10 years; they also may indirectly cause increased dental costs over time because jawbone resorption can change fit and increase oral-health complications. Implants are expensive up front, but with good care, they are much more long-lasting and can be more cost-effective over decades. Real-life affordability often depends on insurance, Medicare (which generally does not cover routine dental), Medicaid (varies by state), dental savings plans, and HSAs/FSAs. For insurance strategies and appeals, see guides on navigating coverage.
2) Dental Implants vs Dentures Timeline & treatment stages
Dental implants — typical sequence and timing
- Consultation & planning: 1–2 visits for exams, X-rays/CBCT scans, treatment plan.
- Pre-treatment (if needed): extractions and/or bone grafting. Extractions heal ~4–8 weeks; bone grafting sometimes requires 3–6 months of healing before implant placement.
- Implant placement surgery: screw (titanium) placed into jawbone. Initial soft-tissue healing takes 7–14 days.
- Osseointegration: the jawbone fuses to the implant — commonly 3–6 months (can be shorter with modern protocols in good bone) before the implant is ready for the abutment/crown. Some protocols (immediate loading or “same day” temporary crowns) exist but are case-dependent.
- Abutment & crown placement: 1–2 visits over a few weeks. Final function achieved after crown placement.
Bottom line: plan on several months from first visit to final crown when no additional surgeries are required; with grafting it can be 6–12 months.
Dentures — typical sequence and timing
- Immediate (same-day) dentures: can be made and placed right after extractions — immediate cosmetic restoration but requires relining as tissues shrink.
- Conventional dentures: if extractions are performed, the dentist often waits 6–8 weeks for gums to heal before final impressions and delivery. Fabrication normally takes a few weeks.
- Adjustment period: most new denture wearers need follow-up appointments for sore spots and relines. Total time from decision to functional denture: from same day (with immediate dentures) up to 6–8 weeks for the most stable fit.
Bottom line: dentures usually allow faster tooth replacement than implants, but achieving a comfortable long-term fit can take several follow-ups.
>>> Watch Video For Dental Health
3) Dental Implants vs Dentures Diet & eating: what to expect after treatment and long-term
Right after implant surgery
- First 24–72 hours: cold liquids, purees, and very soft foods (soups, smoothies, yogurt, mashed potatoes). Avoid hot foods, alcohol, and using straws (to prevent dry socket or disturb clot). Do not smoke — smoking delays healing and raises failure risk. Gradually reintroduce firmer foods over weeks; full chewing capacity returns only after osseointegration and placement of permanent restorations. Many clinicians recommend soft diet for 1–2 weeks and careful chewing patterns for months.
Long-term with implants
- Implants, once restored, allow near-normal biting forces. Seniors with successful implants can chew most foods — which is a major nutritional advantage (better ability to eat meats, raw vegetables, nuts) compared with conventional dentures.
Right after getting dentures
- Initial days–weeks: soft diet recommended — mashed, chopped, or well-cooked foods. Denture wearers should cut food into smaller pieces and chew slowly using both sides of the mouth to stabilize the prosthesis. Adhesives may help but are not a substitute for fit. Taste and temperature perception can change temporarily.
Long-term with dentures
- Many denture wearers can return to a fairly broad diet but often avoid very hard, sticky, or chewy foods (e.g., hard candy, tough steaks, certain nuts). Implant-supported dentures restore much more chewing efficiency than conventional dentures.
4) Dental Implants vs Dentures Health issues, risks, and medical contraindications
Medical conditions that can affect implant success
Dental implants are surgical procedures; systemic health factors that reduce healing or increase infection risk must be considered. Common issues include:
- Uncontrolled diabetes — higher infection risk and slower healing; well-controlled diabetics often do well.
- Active smoking or tobacco use — strongly associated with higher implant failure and delayed healing.
- Radiation therapy to the head/neck — increases risk of osteoradionecrosis; requires specialist input.
- Certain autoimmune diseases or immunosuppressive therapies (e.g., high-dose steroids, biologic agents) — increase risk of complications.
- Bisphosphonate therapy (oral or IV) for osteoporosis or cancer) — particularly IV bisphosphonates can raise risk of medication-related osteonecrosis of the jaw (MRONJ); oral bisphosphonates are a relative/partial contraindication and require careful informed consent and follow-up.
Important: Having one of these conditions does not always exclude implants — many patients with controlled systemic conditions receive implants successfully — but careful medical/dental evaluation and often medical clearance are required.
Age alone is not a contraindication
Chronological age by itself is not a reason to deny implants. Many healthy seniors do exceptionally well with implants; biological age, bone quality, and comorbidities matter more than the number of years lived.
Dentures: risks & health considerations
- Oral sores and tissue irritation: ill-fitting dentures cause sore spots and increase risk of infections like denture stomatitis.
- Bone resorption: conventional dentures do not replace the root, so the jawbone slowly resorbs over time, which changes facial support and fit. This bone loss can make chewing less efficient and make future prosthetic solutions more complex.
- Nutritional risk: poorer chewing efficiency can lead to avoidance of high-fiber, high-protein foods — which matters for seniors at risk of malnutrition.
5) Dental Implants vs Dentures Maintenance and lifetime considerations
Implants
- Daily care: brush and floss like natural teeth; some implant restorations require special floss or interproximal brushes.
- Periodic care: regular dental cleanings and implant checkups (often 2x/year) to monitor bone levels and peri-implant soft tissues.
- Longevity: implants can last decades with good hygiene; however, implant crowns may need replacement after 10–20 years and peri-implantitis (inflammation around implants) can cause loss if not managed.
Dentures
- Daily care: clean dentures daily; remove at night to relieve tissues and reduce denture stomatitis risk.
- Periodic care: relines, rebasing, and adjustments over time; expect at least one reline every 2–3 years for a changing jaw shape. Full replacement often needed every 5–10 years.
- Cost over time: repeated relines/replacements can accumulate cost; also potential dietary and health costs from poorer chewing ability.
6) Dental Implants vs Dentures Who should avoid which option? (Practical guidance)
Who may not be a good implant candidate (or needs caution)
- Uncontrolled systemic disease (e.g., poorly controlled diabetes).
- Heavy smokers unwilling to quit (surgeons typically advise cessation before and after surgery).
- Recent IV bisphosphonate therapy or high risk for MRONJ.
- Severe, untreated periodontal disease or poor oral hygiene that can cause peri-implantitis.
- Insufficient bone that the patient does not want or cannot have grafting to correct (although bone grafts expand candidacy).
- Patients who cannot tolerate oral surgery or general anesthesia due to medical risk — though local anesthesia and sedation options exist.
If you fall into one of these categories, speak openly with your dentist/periodontist and your physician. Many conditions are manageable, and with good control, implant treatment is still possible for many seniors.
Who may not be happy with traditional dentures
- Patients who require high chewing efficiency (e.g., want to eat a broad diet including hard or fibrous foods).
- People highly sensitive to loose prostheses or who find adhesives unacceptable.
- Patients who want to avoid progressive jawbone loss — unless they plan frequent relines/replacements.
Middle ground
- Implant-supported dentures (snap-in overdentures or fixed hybrid prostheses) are often the best compromise for many seniors: they reduce the mobility of dentures, greatly improve chewing, and minimize bone loss compared with removable dentures — while costing less than full fixed implant bridges. These solutions often require fewer implants (2–6 per arch) and can be a sensible “best of both” for many older adults.
7) Dental Implants vs Dentures Practical decision flow for seniors (step-by-step)
- Medical review: review your medical history with both your physician and dentist: diabetes control (HbA1c), medications (bisphosphonates, immunosuppressants), cardiac issues, and clotting medications.
- Oral exam & imaging: panoramic X-ray/CBCT to assess bone volume and sinus proximity.
- Discuss goals and priorities: is maximizing chewing function and bone preservation most important? Or is lower upfront cost and immediate cosmetic restoration the priority?
- Compare options with costs & financing: get itemized quotes: extraction, grafting, implant posts, abutments, crowns, or denture fabrication and follow-up. Ask about payment plans, dental savings plans, and HSA/FSA use. Also explore dental school clinics and community clinics for cost savings.
- Consider hybrid options: implant-retained overdentures can transform denture function with fewer implants.
- Plan for maintenance: understand the follow-up schedule and potential future costs (crowns, relines, hygiene appointments).
8) Dental Implants vs Dentures Nutrition & diet tips for seniors depending on chosen route
After implant surgery (first 1–2 weeks)
- Eat soft, nutrient-dense foods: smooth soups, smoothies (no seeds), mashed sweet potatoes, yogurt, cream-style soups, pureed beans, scrambled eggs. Add protein powders if appetite low. Avoid hot beverages and alcohol for the first 48–72 hours. Avoid straws and smoking.
After receiving new dentures (first few weeks)
- Start with soft chopped foods; cut foods into small pieces; chew gently on both sides of the mouth; avoid sticky and very hard foods until you adjust. Use warm soups and stews for comfort and nutrition. Increase intake of proteins (stewed chicken, soft fish, legumes) and fiber (well-cooked veggies, soft fruits) to avoid nutritional deficits.
Long term recommendations
- Whichever prosthesis you choose, seniors should focus on:
- Adequate protein (to maintain muscle mass and healing ability).
- Calcium & vitamin D for bone health.
- Fiber & hydration for digestive health.
- Soft but varied foods initially; gradually reintroduce more textures consistent with comfort and prosthesis performance.
9) Dental Implants vs Dentures Final recommendation — how to choose
- If you are medically healthy or have controlled chronic conditions, want long-term chewing power, and can manage the upfront cost or financing → implants (or implant-supported prosthesis) are usually the best option for function, bone preservation, and long-term satisfaction.
- If you need fast restoration, have limited funds, or cannot undergo oral surgery due to medical constraints → conventional dentures are a valid, practical solution that restores appearance and some chewing ability; consider implant-supported overdentures if you want improved stability and can place a few implants.
- If you’re between those extremes, ask about implant-retained (snap-in) dentures — they often dramatically improve stability and diet for seniors while requiring fewer implants than full fixed bridges.
10) Dental Implants vs Dentures Frequently Asked Questions (FAQ)
Q: Will implants fail because I’m old?
A: Age alone is not the primary risk factor. General health, bone quality, smoking, and hygiene are the main determinants. Many seniors over 70 and 80 successfully receive implants.
Q: How long until I can eat normally after an implant?
A: You’ll be on a soft diet for days to weeks post-surgery and should avoid heavy chewing on the implant until osseointegration is complete (commonly 3–6 months), unless your clinician has used an immediate-load protocol.
Q: Are implant teeth painful?
A: Implant surgery involves post-op discomfort like any oral surgery, but pain is typically well-managed with prescribed or over-the-counter medications and subsides in days to weeks.
Q: Can Medicare help pay?
A: Traditional Medicare generally doesn’t cover routine dental care, including implants and dentures, though certain Medicare Advantage plans or Medicaid (for eligible beneficiaries in some states) may cover parts or offer dental add-ons. Check plan details and ask dental offices about billing alternatives.

